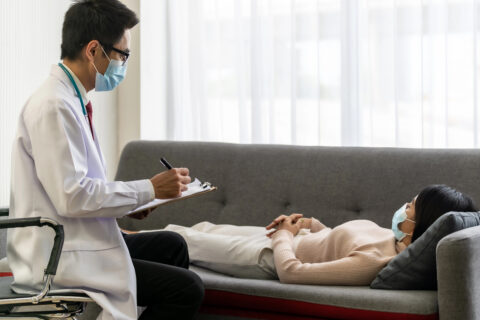
Dual diagnosis is a treatment method that addresses the complex relationship between mental health disorders and substance use disorders (SUDs). Dual diagnosis treatment helps patients avoid relapse by focusing on the big picture of wellness.
Understanding Dual Diagnosis
According to the 2021 Substance Abuse and Mental Health Services Administration (SAMHSA) survey, over 9 million adults in the United States have a co-occurring disorder. A co-occurring disorder occurs when a person has a mental illness and a substance use disorder at the same time. Per SAMHSA, no specific combinations of SUDs and mental health disorders are required to qualify under the parameters of what is considered a dual diagnosis.
Instead, any number of examples that may occur and co-occur. For example, any of the typical substances in illicit and prescription drugs can fall under SUD, including:
- Alcohol
- Benzodiazepines
- Methamphetamine
- Opioids like fentanyl and heroin
Mental Health Disorders in Dual Diagnosis
Mental health disorders may also vary widely in the case of a dual diagnosis, and it is often the case that patients can experience more than one well. Common examples include:
- Attention deficit hyperactivity disorder (ADHD)
- Post-traumatic stress disorder (PTSD)
- Bipolar disorder
- Schizophrenia
- Anxiety
While mental health and substance abuse may have once been separate topics, ongoing medical research shows how they are connected. However, developing that mindset from a treatment perspective first requires that mindset in the diagnosis phase. That’s where dual diagnosis comes into play and why it can significantly improve patients’ treatment.
Importance of Addressing Mental Health and Substance Abuse Together
Dual diagnosis treatment is a specialized approach because it addresses mental health disorders and substance abuse concurrently. This essential treatment recognizes the connection between these two aspects, and the result is that dual diagnosis treatment can provide a holistic and effective approach to recovery.
It’s crucial to treat both conditions at the same time because they often worsen each other. Ignoring one aspect can lead to an incomplete recovery and a higher risk of relapse. Fortunately, the medical community recognizes the importance of dual diagnosis.
Exploring the Correlative Relationship of Dual Diagnosis
According to MedlinePlus, around 50% of people who either have a mental health disorder or SUD will have the other either simultaneously or at some other point in their lives. What’s more, there is a direct link between mental health disorders and SUDs. Each one plays into the other, worsening symptoms in a vicious cycle.
In some ways, understanding this relationship can be difficult. On the one hand, it can be assumed that someone with an SUD may go on to develop a mental health disorder due to the impact of withdrawal symptoms.
Substance Abuse and Addiction
Some people may not have been diagnosed with a mental health disorder such as anxiety or depression before developing an addiction. For example, if a person who is addicted to Xanax tries quitting the drug on their own, they could experience acute anxiety and other withdrawal symptoms.
Now, they are caught in the vicious cycle of co-occurring disorders with drug misuse and addiction, the mental health condition of anxiety, and the Xanax-related substance use disorder. This example is certainly plausible, but it is not the only example of how co-occurring disorders occur in a dual diagnosis.
The Treatment Process for Dual Diagnosis
The first step in dual diagnosis treatment is undergoing a thorough assessment to identify the specific mental health disorders and the extent of substance abuse. This assessment forms the basis for a tailored treatment plan.
It is important to note that dual diagnosis is a treatment approach that addresses issues in a particular order. To go back to our earlier example, if someone is struggling with anxiety and a Xanax addiction, it is important to determine which came first and if it is possible to determine that in the first place. However, that kind of introspection comes later in the treatment process. Before determining which disorder gave rise to the other, a dual diagnosis will be primarily concerned with properly identifying both disorders.
Integrated Treatment Approach
Dual diagnosis treatment is comprehensive, particularly since it typically accompanies detox programs at residential treatment centers before moving into outpatient therapy. This means that overall, dual diagnosis treatment is an integrated approach that often combines medication to manage mental health symptoms with therapy to address behavioral issues and addiction. This dual approach is crucial for effective treatment.
The Role of Psychotherapy
Psychotherapy, including cognitive behavioral therapy (CBT) and group therapy, is vital in helping individuals understand their behaviors and develop coping strategies. One study shows that cognitive behavior therapy is considered one of the most effective treatment strategies today, calling it “the gold standard.”
Ongoing support from family and friends is critical in dual diagnosis treatment. This support helps individuals begin treatment, maintain their recovery, and manage their mental health in the long term. Substantial medical evidence identifies isolation as a contributing factor to many disorders. Surrounding individuals with love and family-focused support practices can counteract isolation from playing a role in preventing relapse.
Challenges in Dual Diagnosis Treatment
Stigma and misconceptions about mental health and addiction can be significant barriers to seeking treatment. Education and awareness can help overcome these challenges.
An effective way to develop awareness is by hearing from those who have successfully navigated dual diagnosis treatment, which can be incredibly motivating. These stories offer hope and a sense of hope. Staying hopeful and persistent is crucial in the recovery journey.
Choosing the Right Treatment Facility for Dual Diagnosis Treatment
When selecting a treatment facility for dual diagnosis therapy, you should consider factors like:
- The staff’s experience
- The therapies offered
- The facility’s approach to dual diagnosis treatment
Ask about the facility’s accreditation, success rates, and aftercare support to ensure its treatment program meets your needs. Dual diagnosis treatment is a comprehensive approach that addresses the intertwined issues of mental health disorders and substance abuse. It offers hope and a recovery pathway for those with these co-occurring conditions.
If you or someone you know is struggling with a co-occurring disorder, it’s crucial to seek professional help to receive an accurate dual-diagnosis treatment approach. The right treatment can lead to a fulfilling, sober life.
Frequently Asked Questions (FAQs)
How Is Dual Diagnosis Treatment Different From Other Addiction Treatments?
Dual diagnosis treatment focuses on the connection between substance use disorder (SUD) and adverse mental health conditions.
How Long Does Dual Diagnosis Treatment Typically Take?
It depends. Treatment will often accompany a detox program for a substance use disorder (SUD), with residential and outpatient treatment playing a key role in patients’ lives, helping them maintain recovery and wellness. Treatment will generally continue for several months, and medical professionals can modify treatment timelines according to each patient’s needs and progress.
Can Family Members Get Involved in the Treatment Process?
Yes. Family members should always recognize their key role in love and support for family members undergoing treatment. Beyond this crucial role, they could join group therapy settings, depending on the mental health disorder(s) a patient has.
Sources
- Substance Abuse and Mental Health Services Administration. (2023 July 26). Co-Occurring Disorders and Other Health Conditions. Retrieved from: https://www.samhsa.gov/medications-substance-use-disorders/medications-counseling-related-conditions/co-occurring-disorders#:~:text=According%20to%20SAMHSA’s%202021%20National,can%20have%20serious%20adverse%20effects. Accessed on July 14, 2025.
- Substance Abuse and Mental Health Services Administration. (2022). Key Substance Use and Mental Health Indicators in the United States: Results from the 2021 National Survey on Drug Use and Health. Retrieved from: https://www.samhsa.gov/data/sites/default/files/reports/rpt39443/2021NSDUHFFRRev010323.pdf. Accessed on July 14, 2025.
- MedlinePlus. (n.d.). Dual Diagnosis. Retrieved from: https://medlineplus.gov/dualdiagnosis.html. Accessed on July 14, 2025.
- Health Direct. (2022 August). Addiction Withdrawal Symptoms. Retrieved from: https://www.healthdirect.gov.au/addiction-withdrawal-symptoms. Accessed on July 14, 2025.
- National Institute on Drug Abuse. (2020 July). Drug Misuse and Addiction. Retrieved from: https://nida.nih.gov/publications/drugs-brains-behavior-science-addiction/drug-misuse-addiction. Accessed on July 14, 2025.
- National Library of Medicine. (2018 January 29). Why Cognitive Behavioral Therapy Is the Current Gold Standard of Psychotherapy. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5797481/. Accessed on July 14, 2025.
- National Library of Medicine. (2018 January 13). Family-focused practices in addictions: a scoping review protocol. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5781095/. Accessed on July 14, 2025.
Facility Staff
November 27, 2023
- Mental Health Residential Treatment in North Carolina
 When managing life starts to feel like the whole job, what’s the next step? A clear look at residential mental health care in NC.
When managing life starts to feel like the whole job, what’s the next step? A clear look at residential mental health care in NC. - Online IOP Program North Carolina
 What if distance was never the real barrier to mental health care in North Carolina? See how online IOP is changing access across the state.
What if distance was never the real barrier to mental health care in North Carolina? See how online IOP is changing access across the state. - Online IOP Program Georgia
 You look fine on the outside. But what happens when that quiet weight never lifts? See how an online IOP in Georgia helps without putting your life on hold.
You look fine on the outside. But what happens when that quiet weight never lifts? See how an online IOP in Georgia helps without putting your life on hold. - Mental Health Therapy Program North Carolina
 Not all mental health care works the same. So how do you know which approach actually fits you?
Not all mental health care works the same. So how do you know which approach actually fits you? - Mental Health Rehab North Carolina
 Why do so many people treat one problem… while another silently keeps them stuck?
Why do so many people treat one problem… while another silently keeps them stuck? - Mental Health Hospital North Carolina
 Searching for a mental health hospital North Carolina? Discover why Otter House Wellness is the trusted choice for simple and personalized family care.
Searching for a mental health hospital North Carolina? Discover why Otter House Wellness is the trusted choice for simple and personalized family care. - Drug Rehab North Carolina
 Searching for drug rehab North Carolina? Learn how specialized, veteran-focused care at Otter House Wellness can help you move from survival to stability.
Searching for drug rehab North Carolina? Learn how specialized, veteran-focused care at Otter House Wellness can help you move from survival to stability.
Recommended Blogs


Mental Health Residential Treatment in North Carolina

Online IOP Program North Carolina